Physiological Sciences
The Physiological Sciences comprise Audiology, Gastrointestinal and Neurophysiology.
Audiology
Healthcare Scientists in Audiology see patients to test their hearing and balance. They prescribe and maintain hearing aids programmed to their individual hearing loss, meeting their hearing needs using complex computer programmes that set the hearing aids to optimise hearing ability.
Specialists in Audiology also identify causes of balance disorders and deliver a range of treatment options to cure or improve balance and dizziness. They also see patients with tinnitus (often described as a buzzing or whistling in the ear) and offer a range of management options including therapy-based approaches.
Audiology covers all ages from newborns to centenarians.
Watch Heather talk about the work of a Senior Audiologist:
Hear about Dan’s experience of working as a third-year STP student in Audiology:
Gastrointestinal Physiology
The Norfolk Physiology Unit provides a gastrointestinal (GI) diagnostic physiology service for Norfolk and Suffolk.
Meet the team

The team comprises:
- Yvette Wright, Lead Gastrointestinal (GI) Physiologist
- Oliver Smith, GI Physiologist
- Jane Bunyan, Senior Nurse specialist in Urodynamics
- Lisa Wright, Senior Healthcare assistant
- Susanne Nash, Clerical Officer
- Brandon Karn, Receptionist
- Lily Warner, Receptionist.
Services
The Norfolk Physiology offers the following investigations:
- High-resolution manometry – a test to assess swallowing
- 24-hour pH, 24hr pH/impedance tests and 96hr Bravo tests – tests to assess acid reflux and indigestion
- Anorectal physiology tests – tests to look at the strength of the muscles in the anal canal
- Biofeedback – teaching bowel retraining for constipation
- Irrigation – a treatment taught for constipation and faecal incontinence
- Urodynamics video and Ambulatory Urodynamics – to look at how the bladder works.
Patients are referred for high-resolution manometry and 24-hour pH tests if they have difficulty swallowing, a persistent cough, heartburn or chest pain, nausea and vomiting.
The manometry test assesses swallowing – watch this video from Hull Hospital to see how.
24hr pH tests are undertaken after HRM to assess acid reflux over a 24-hour period with the patient off antacid medication. It can also be used with a patient on antacid medication to see if the medication works to stop acid reflux
Watch the video below to see Dr Ruth Doherty Consultant Urologist, explain our NPU Urodynamics service. https://share.icloud.com/photos/07cfxmdG4kkepoiS_ixTPclCw#Norfolk_and_Norwich_University_Hospitals_NHS_Foundation_Trust
Gastrointestinal Physiologist training
To become a GI Physiologist you need to study for a degree and an MSc in Clinical Science (Physiological Sciences) MSc (Scientific Training Programme). See details about this course at Newcastle University.
There’s also a practical pathway called the Accredited Specialist Scientific Practice (ASSP) route with the Academy of Healthcare Science at Newcastle University. For this pathway, you need to be already employed as a trainee Physiologist with a Physiology degree or equivalent and a previous background as a healthcare professional or Nurse. Training is provided under supervision by the Senior Physiologist as well as examinations at Newcastle University.
All GI Physiologists need to be registered with the Association of GI Physiologists (AGIP) when qualified. Find out more.
Watch Yvette Wright explain the work of a Healthcare Scientist in Gastrointestinal Physiology and the training route:
Clinical Neurophysiology
Healthcare Scientists in Neurophysiology investigate the function of nerves to diagnose and monitor neurological disorders using complex computer equipment to record electrical activity from the brain or other nerves within the body.
As well as their own clinics, they work alongside doctors in theatre for nerve monitoring during surgery.
Watch Trainee Healthcare Scientist Briony talk about her route into Neurophysiology:
Clinical Neurophysiology provides an array of neurophysiological investigations to a diverse range of patients. On average, we see around 5,500 patients a year and our team comprises eight Scientists, two Consultant Neurophysiologists, a Locum Doctor in Neurophysiology and three administrative staff.
The investigations we offer include:

EEG (ElectroEncephaloGram): This is a recording of the electrical activity produced by the brain performed by applying around 23 electrodes to the scalp. Recordings routinely last for 20 minutes, but may go on for an hour for a sleep recording or a day or more if we are trying to capture some of the patient’s symptoms.
It is typically used to test for epilepsy/seizures and also encephalopathy (dysfunction of the brain), ranging from CJD to hepatic encephalopathy. Video is normally recorded at the same time to capture clinical symptoms. It is painless, but leaves the patient with a sticky head. It is performed and reported by the scientists and the Consultant Neurophysiologist provides the clinical interpretation of the result.

Nerve Conduction Studies: These provide an assessment of peripheral nerve function, performed by applying an electrical stimulus to a nerve via electrodes placed in one location (eg a finger), producing a response in the nerve which is recorded from some electrodes placed further along the nerve (eg the wrist).
From this we can reveal the speed of the response (this tells us about the coating of the nerve, the myelin) and the size or amplitude of the response (which shows how the individual fibres that make up a nerve, the axons, are working). By testing nerves in different places we can look at the pattern of the results to tell if there is a problem with a nerve in one location (as seen in Carpal Tunnel Syndrome) or if the nerves are generally not working normally (eg a peripheral neuropathy).
It’s performed and reported by the scientists or the Consultant Neurophysiologist, who provides the clinical interpretation of the result.
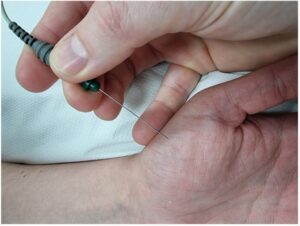
EMG (ElectroMyoGraphy): This is a recording of the electrical activity produced by the muscles to look for disorders of the muscles and the nerves that supply them.
The investigation is normally performed in conjunction with nerve conduction studies. It is recorded by inserting a needle electrode into a muscle and getting the patient to activate or tense that muscle. It’s only performed and interpreted by the Consultant Neurophysiologist and is useful in the diagnosis of a range of conditions, including nerve palsies, Myasthenia Gravis, Muscular Dystrophy, nerve root disorders or motor neurone disease.
Evoked Potentials: A group of tests that examine different sections of neuroanatomy by presenting a stimulus to the patient and recording a response.

VEP (Visual Evoked Potential): This tests the visual systems and ultimately the optic nerve. It is performed by presenting a visual stimulus to the patient (an alternating pattern on a screen), which produces a response in the brain that’s recorded from electrodes placed over the back of the head. It is useful for detecting problems with the central nerves (such as Multiple Sclerosis) or investigating problems with vision.

ERG (ElectroRetinoGraphy): This looks at the retina, the cells at the back of the eye which turn the light from everything in our vision into electrical signals which are passed to and processed by the brain. It is performed by presenting a visual stimulus to the patient (an alternating pattern on a screen or a flashing light). The electrical signal produced by the retina is then recorded from some special electrodes placed under the bottom eyelid. It is useful for detecting various eye diseases, such as Retinitis Pigmentosa, night blindness or cancer-associated retinopathy.

SEP (Somatosensory Evoked Potentials) assess a whole sensory nerve pathway by stimulating a nerve with electrical stimulus and recording the resultant response as it passes through different parts of the neuroanatomy. For example, we might stimulate a nerve at the ankle, record the response from the nerve at the back of the knee, then from the lower back as the nerve passes into the spinal cord and from the brain via electrodes placed on the scalp. It is often used to functionally assess a nerve pathway for disorder and to distinguish between problems with a peripheral nerve (eg a nerve palsy in the arm or leg) and a central nerve (eg Multiple Sclerosis).
All of the Evoked Potentials are performed and reported by the scientists and the Consultant Neurophysiologist provides the clinical interpretation of the result.
Intra Operative Monitoring (IOM): This employs a range of evoked potentials during Orthopaedic Spinal Surgery to look out for collateral damage to the spinal cord which may occur as a consequence of the surgery. Prompt detection of such complications during the operation potentially allows them to be reversed and for the surgery to be optimised. It is performed, interpreted and reported by the scientists.
Training routes in Neurophysiology
There are a number of routes that mirror those available within all of Healthcare Science, including apprenticeships, Practitioner Training Pathway (PTP), Scientist Training Pathway (STP), Accredited Scientific Practice Programme (ASP) and Higher Specialist Scientist Training Programme (HSST).
Apprenticeships: This route is available to GCSE and A-Level (or equivalent) students. Candidates normally apply for an apprentice position offered by a Neurophysiology department. The training involves completion of a level 2 or 4 Healthcare Science Diploma funded by the employer. It typically takes four to five years to complete. This route acts as a gateway into a career in Healthcare Science at an Assistant.
PTP: This is a three-year BSc (Hons) undergraduate training programme that includes work-based and academic learning. Applications are open to A-Level students via UCAS – it’s a “self-funded” course. On completion, individuals are able to apply for vacancies and pursue a career as a Healthcare Science Practitioner in Neurophysiology, performing EEG investigations.
STP This is a three-year programme of work-based learning, supported by a university accredited Master’s degree. Entry is open to individuals who have a First or 2.1 in an Honours degree or a 2.2 with a relevant Master’s degree in a pure or applied science. The applications process is competitive.
Successful candidates are awarded a fixed-term training contract salaried at AfC Band 6 (at a Neurophysiology department) and will attend university to complete the fully-funded part-time Master’s degree. On completion, individuals are eligible for statutory Clinical Scientist registration (with the HCPC) and apply for Clinical Scientist roles in Neurophysiology.
ASP: This route is available to individuals holding a First, 2.1, or 2.2 Honours degree in a pure or applied science. Candidates normally apply for a training position offered by a Neurophysiology department (often salaried at AfC Band 4). The training involves completion of a Post Graduate Certificate (this can be expanded to an MSc) that is comprised of modules taken from the STP programme. This is augmented by on-the-job training and assessment (see below) and is delivered and all funded by the employing Neurophysiology department. It typically takes three to four years to complete and qualifies the individual to perform all standard investigations (EEG, NCS and VEPs). At this point, they typically progress to an AfC Band 6.
HSST: This is a five-year, work-based training programme that provides opportunities for qualified and experienced clinical scientists to train to become eligible to apply for available consultant clinical scientist posts. It is supported by a Doctoral level academic award.
The PTP, STP and ASP routes can be augmented by the trainee also completing two professional body examinations. These are provided by the Association of Neurophysiological Scientists (ANS). One examination covers EEG and the other encompasses Nerve Conduction Studies and Evoked Potentials.
For each of the two exams, the student produces a portfolio that includes a number of work-based assessments, evidence of experience and five case studies. The student then undergoes a practical assessment where they conduct the investigation in their workplace. This is assessed by two external assessors, who are themselves Healthcare Scientists in Neurophysiology from other Hospitals. They will also mark the portfolio and ultimately give the final outcome of whether the student was successful.
Further information
www.ansuk.org
@ClinNeurophys
www.bscn.org.uk
www.neuromonitoringuk.org
www.nhsemployers.org
www.nshcs.hee.nhs.uk
www.ahcs.ac.uk
Contact us
Adrian Tearle, Lead Healthcare Scientist in Neurophysiology
Clinical Neurophysiology,
Norfolk & Norwich University NHS Trust
Colney Lane
Norwich NR4 7UY
Email: adrian .tearle@nnuh.nhs.uk


